We all know that Covid-19 is a respiratory illness and you catch it by inhaling infected droplets, but can the virus that causes it (SARS-CoV-2) be found in wastewater and if so is that a good or a bad thing?
Spread of Covid-19 in water
SARS-CoV-2 has been detected in the faeces of some patients diagnosed with the disease, although the amount of virus shed in stools, for how long the virus is shed, and whether the virus in stools is infectious is not yet known. The risk of transmission of the virus from the faeces of an infected person is also unknown. However, that risk, based on data from previous outbreaks of related coronaviruses, such as severe acute respiratory syndrome (SARS) and Middle East respiratory syndrome (MERS) is expected to be low. And there has been no confirmed faecal-oral transmission of Covid-19 to date (April 29th 2020).
SARS-CoV-2 has already been detected in wastewater, though just to be clear, not in drinking water and conventional water treatment methods, such as filtration and disinfection, should remove or inactivate it. There is also no evidence that Covid-19 can be spread to humans through the use of pools, hot tubs or spas, or water playgrounds.
Ok, so it doesn’t seem such a bad thing…. But is it a good thing? Could this discovery help in stopping the spread of infections in any way? Could it be used to measure the effectiveness of interventions such as social distancing?
Most countries have controlled the unchecked spread of Covid-19 by lockdown of their populations, South Korea, Hong Kong and Sweden being three of the few countries which haven’t gone down that route. But lockdown causes severe economic and social problems and a route out of it, whilst still controlling the spread of the virus, needs to be found.
A second wave of infections
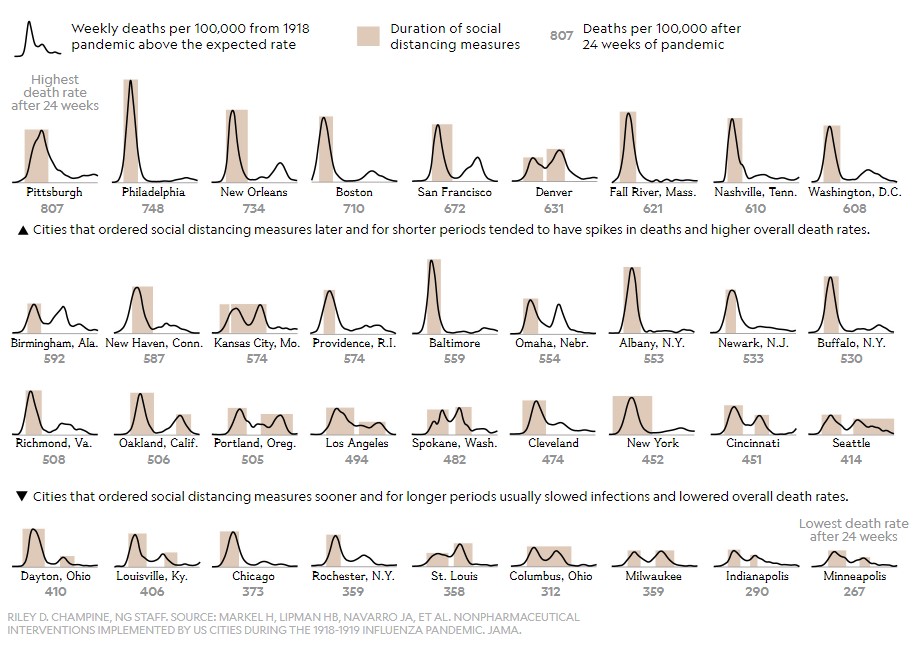
As countries start to come out of lockdown and lift social distancing measures the effect of the severity of a second wave of infections is unknown. Is one likely to happen? Probably. Figures vary but the 1918 Spanish flu pandemic killed an estimated 50 million people worldwide and occurred in multiple waves, with the latter waves often more severe than the first. This pattern has been replicated in subsequent flu pandemics. How and why multiple-wave outbreaks occur is not clear, and therefore how subsequent waves of infection can be prevented, also does not have a straightforward solution (as demonstrated by this series of graphs showing number of cases and lock down periods for all major US cities during the Spanish flu pandemic).[1]
But it is clear that it would obviously be preferable to track and stop any second wave as soon as possible. And it is here where the presence of SARS-CoV-2 in wastewater becomes a good thing.
Testing wastewater
Testing wastewater could be used as a way to find clusters of Covid-19 outbreaks more quickly than clinical testing of suspected cases. It would also help to mitigate the global shortage (and reliability in some cases) of test kits for individuals. More than a dozen research groups worldwide have started analysing wastewater as a way to estimate the total number of infections in a community.
The ability to track infectious diseases that are excreted in urine or faeces is not new technology. Wastewater monitoring has been used for decades to assess the success of vaccination campaigns against poliovirus, and in the Netherlands more recently it has been used to detect outbreaks of norovirus, antibiotic-resistant bacteria, poliovirus and measles. The Netherlands National Institute for Public Health and the Environment detected traces of SARS-CoV-2 in wastewater at Schiphol Airport in Tilburg only four days after the Netherlands confirmed its first case of Covid-19 using clinical testing. They also found viral RNA of SARS-CoV-2 in the city of Amersfoort before infections had been reported in the community.
In Queensland, scientists were quick to start testing for SARS-CoV-2 in wastewater and were able to detect a gene fragment of the novel coronavirus in untreated sewage from two wastewater treatment plants. It’s not a surprise that Australia, along with the Netherlands, are currently at the forefront of this research. The country enforced a stringent lock down when they had very few cases and at the time of writing (29th April 2020) have just 6,649 cases and 74 deaths – a rate of just 3 deaths per 1m population.[i] What the country does not want is an unchecked and severe second wave of cases once the lockdown is lifted, hence their search for a fast way to test multiple people at one time.
Studies in China have shown that SARS-CoV-2 can appear in faeces within three days of infection, which is much sooner than the time taken for people to develop symptoms severe enough for them to seek hospital care — up to two weeks — and get an official diagnosis and also quicker than many cases are being detected with conventional tests. Therefore, routine wastewater testing could be used as a non-invasive early-warning tool to alert communities to new Covid-19 infections, before the disease has been picked up through individuals showing symptoms or before they have been tested. Tracking viral particles in wastewater could give information about an outbreak seven to ten days in advance which would make a lot of difference in the subsequent severity of any particular outbreak.
A large single treatment plant can capture wastewater from hundreds of thousands of people so monitoring its influent tests, in effect, a wide number of people in one go. At this scale, sewage sampling would be able to detect the approximate number of people infected in a geographic area without testing every individual, thus allowing new outbreaks to be quickly identified. Sewage sampling could be conducted daily, and if the tests at the wastewater treatment plant was positive there is the potential to take sampling “further up the pipe” to a suburban level by taking samples from branch drain pipes, thus isolating the source of a breakout to smaller populations who can them be clinically tested.
There is still some research to be done however. To quantify the scale of infection in a population from wastewater samples, researchers will need to find out how much viral RNA from SARS-CoV-2 is excreted in faeces, and extrapolate the number of infected people in a population from concentrations of that RNA in wastewater samples. They also need to ensure that their tests can detect the virus at low concentration levels. And it’s important that wastewater surveillance, should it be feasible, does not take away resources from the clinical testing of individuals.
[1] https://www.nationalgeographic.com/history/2020/03/how-cities-flattened-curve-1918-spanish-flu-pandemic-coronavirus/
[2] https://www.worldometers.info/coronavirus/#countries
The following websites were also accessed to inform this article:
https://www.nature.com/articles/d41586-020-00973-x
https://www.cdc.gov/coronavirus/2019-ncov/php/water.html
https://www.theguardian.com/world/2020/apr/20/will-there-be-second-wave-of-coronavirus-